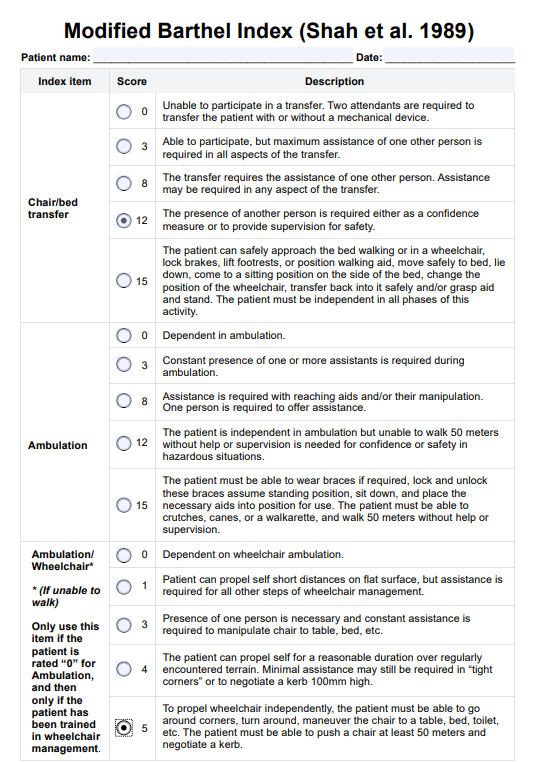
The modified barthel index is more than a simple checklist of daily activities—it is a structured clinical framework used to quantify functional independence with measurable precision. While most resources focus on basic scoring, deeper understanding of its scoring logic, weighting system, and clinical interpretation reveals its true value in rehabilitation and long-term care.
A modified barthel index pdf is not just a printable form; it acts as a standardized decision-making tool that helps clinicians evaluate recovery patterns, predict outcomes, and design personalized care plans.
Use Modified Barthel index Calculator
Advanced Understanding of the Modified Barthel Index
The modified barthel index (MBI) is built on the principle that independence is not binary. Instead of simply marking tasks as “done” or “not done,” the MBI evaluates levels of assistance required, capturing subtle differences in patient ability.
Key Concept:
Each activity is scored based on:
- Complete independence
- Supervision or minimal help
- Partial assistance
- Full dependence
This layered scoring allows the scale to detect even small improvements, which is critical in rehabilitation settings such as stroke recovery.
Hidden Scoring Logic (What Most Resources Don’t Explain)
Most basic guides list activities and scores, but the real strength of the modified barthel index scale lies in its weighting system.
1. Weighted Functional Importance
Not all activities are scored equally.
- Mobility and transfers carry higher weight
- Grooming and bathing carry lower weight
This reflects real-life independence—being able to move independently impacts quality of life more than minor self-care tasks.
2. Time-Based Independence Factor
Scoring indirectly considers:
- Time taken to complete a task
- Efficiency of movement
- Need for rest or assistance
A patient who completes a task slowly but independently may score higher than one who needs help but finishes quickly.
3. Safety Awareness Component
Although not always explicitly stated, clinicians often factor in:
- Risk of falls
- Balance stability
- Cognitive awareness during tasks
This adds a clinical judgment layer beyond the raw score.
Modified Barthel Index Score Interpretation (Beyond Basics)
Standard score ranges are useful, but deeper interpretation provides more clinical insight.
Functional Meaning of Scores:
- 0–20 (Total Dependency)
Requires full-time care; minimal self-function - 21–60 (Severe Dependency)
Limited participation; high caregiver involvement - 61–90 (Moderate Dependency)
Can perform several tasks independently but needs support for mobility or complex activities - 91–99 (Near Independence)
Minor assistance or supervision required; often safe for home discharge with support - 100 (Full Independence)
Complete functional autonomy
Advanced Insight:
A 10-point improvement is often considered clinically significant in rehabilitation, especially in stroke patients.
Modified Barthel Index vs Real-Life Independence
A common misconception is that a high score always equals full independence.
Important Reality:
- A patient with 95 score may still struggle in unfamiliar environments
- Environmental factors (stairs, uneven surfaces) are not fully captured
- Cognitive and emotional factors are not directly measured
This is why clinicians use the MBI alongside other tools.
Modified Barthel Index Calculator (Professional Use Insight)
While a modified barthel index calculator simplifies scoring, expert users rely on it differently:
- Used for baseline vs follow-up comparison
- Helps identify plateau in recovery
- Supports data-driven rehabilitation planning
Advanced Tip:
Tracking scores over time (trend analysis) is more valuable than a single score snapshot.
Clinical Applications You Won’t Find in Basic Guides
1. Predicting Hospital Discharge
Patients scoring above 90 are often considered for home discharge with minimal support.
2. Stroke Rehabilitation Benchmarking
Used to measure:
- Rate of recovery
- Effectiveness of therapy interventions
3. Insurance & Care Planning
Scores are sometimes used to:
- Justify need for continued therapy
- Determine level of home care services
4. Elderly Functional Decline Monitoring
Small score drops (5–10 points) can indicate:
- Early health deterioration
- Increased fall risk
Limitations of the Modified Barthel Index
No tool is perfect, and understanding limitations adds depth to its use.
- Does not assess cognitive function
- Limited sensitivity at higher scores (ceiling effect)
- Does not account for environmental challenges
- Relies partly on observer judgment
Because of this, it is often combined with other assessments like functional independence measures.
What Makes a High-Quality Modified Barthel Index PDF?
Not all PDFs are equally useful. A well-designed modified barthel index 0–100 pdf should include:
- Clearly defined scoring criteria for each activity
- Weighted scoring system (not just checkboxes)
- Instructions for consistent assessment
- Space for longitudinal tracking (multiple dates)
- Interpretation guide integrated into the sheet
Advanced Addition (Recommended for Your PDF):
- Progress tracking table (Week 1, Week 2, Week 3)
- Notes section for clinical observations
- Risk indicators (fall risk, assistance level)
This transforms a basic form into a professional assessment tool.
Practical Example (Real-World Scenario)
A patient recovering from stroke:
- Week 1 score: 35 (Severe dependency)
- Week 4 score: 65 (Moderate dependency)
- Week 8 score: 92 (Near independence)
Interpretation:
- Strong rehabilitation progress
- Likely ready for discharge with minimal assistance
- Continued outpatient therapy recommended
This type of progression tracking is where the modified barthel index becomes truly powerful.
Conclusion
The modified barthel index is not just a scoring sheet—it is a clinically meaningful system for understanding human independence in measurable terms. When used beyond basic scoring, it becomes a powerful tool for tracking recovery, guiding treatment, and improving patient outcomes.
A well-structured modified barthel index pdf free download combined with proper interpretation can significantly enhance assessment accuracy and care planning.
FAQs
1. What makes the modified barthel index different from simple ADL checklists?
It measures levels of assistance and uses weighted scoring, providing a more detailed and clinically useful assessment.
2. Is a higher score always better in real-life situations?
Not always. Environmental and cognitive factors can still affect independence despite a high score.
3. How often should the modified barthel index be assessed?
It is typically reassessed weekly or during key stages of rehabilitation to track progress.
4. Can the modified barthel index predict recovery outcomes?
Yes, trends in scores over time can help predict rehabilitation success and discharge readiness.
5. Why is mobility weighted more heavily in the scoring system?
Because mobility directly impacts overall independence and ability to function in daily life.